The new healthcare system
As far as that is still new...
Do you recognize that feeling of getting stuck in terms that have long since faded away? I experience this with our current healthcare system. In a rush, I still refer to it as 'the new healthcare system.' Quite strange, really. The system has been in place since 2006 and is no longer so new. Moreover, it is rather opportunistic when you consider the term itself; am I, with this Freudian slip, actually calling for a new healthcare system deep down in my heart? I believe that a new system or a substantial adjustment to our current system is not far from what we need now.
The current system brings many positives. But as often happens with systems, over time it tends to undermine itself. This is also happening now with our current DBC system. What was once conceived as well-balanced and supportive is beginning to show significant cracks. More than ever, it’s about providing and paying the lowest premium, and beyond that, it seems to matter less to everyone. Until you find yourself in need of care!
The current system is based on roughly three principles:
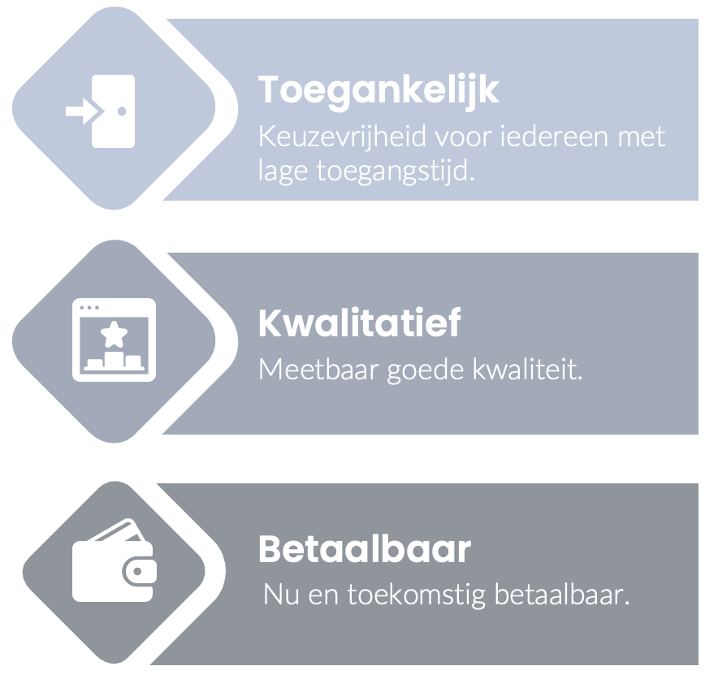
The image has not been translated from the original language, Dutch. The context is further explained below.
I will not write an essay on the extent to which each point has or has not been addressed. However, I would like to highlight the striking aspects that have been well addressed and the points that have not been as successful. I will touch on a few points that, in my opinion, should form the subject of discussion when considering a change to the system. This is because they have such a significant impact on what is currently not going well.
Cost prices, selling prices, and market prices
Since the inception of the current healthcare system, its structure has been heavily focused on controlling costs. If we were to know exactly what healthcare would cost, we could purchase it as business products and goods. It must be said; after the decline in the number of DBCs (approximately 44,000) to DOTs (around 4,000), there was at least a more manageable number of diagnoses that could be contracted. Initially, prices were still primarily calculated in a rough manner. Only after a considerable amount of time did contracting take on more form as cost calculations began to acquire a normative structure. This has not always happened explicitly, but it has indeed occurred.
"Has the quality of care deteriorated? Has the value of care diminished?"
For now, however, the focus on pricing is no longer of great significance. At least, not in a real sense. Many prices that are now agreed upon as 'rates' are accompanied by mandates from insurers to fit these within the percentile of the x-best rates. A true race-to-the-bottom. Has the quality of care diminished? Has the value of care decreased? No, that is not the story, in my opinion. This action is still taking place because the insurance premium must remain affordable. Instead of focusing on the affordability of care itself, the emphasis is primarily on acquiring more insured individuals. This is a strange phenomenon, especially as the negative effects of this trend are becoming increasingly pronounced within healthcare organizations. It is becoming increasingly difficult for them to absorb financial fluctuations, attract external capital, and make the necessary investments. The core question, as far as I am concerned, is: are we still searching for rate pressure, or have we already shaped the means to create price pressure, but must actual cost control come from elsewhere?
Risk premiums and system funds
From the moment a health insurer gains more insured individuals, its market power increases. This can be more manageable for a healthcare provider, as it does not have to make various agreements with more insurers that hold a substantial market share (and that differ in their policies). It is important to note that at the time of writing, there are 10 insurers in the Netherlands with whom hospitals must make agreements; 10! Internally managing policies becomes easier with the acquisition of a larger market share by a health insurer. After all, it remains very difficult to explain (and moreover undesirable) why insured individuals from insurer X can be helped within a certain timeframe while those from insurer Y cannot. This kind of steering is far from desirable. This card is not often played by healthcare providers, although there is some bluffing involved, which should not be necessary.
Okay, more market power due to the fluctuations in the number of insured individuals can be beneficial, but what happens then? It introduces an inequity in the system costs among insurers. Based on the number of insured individuals that the insurer covers, it must maintain reserves. This obligation arises from the provisions of Solvency II. However, the reserves that the insurer maintains do not transfer from the outgoing to the incoming insurer. This represents pure profit in terms of solvency for the outgoing insurer. It also leads to the accumulation of a new reserve at the incoming insurer, resulting in a double loss for healthcare.
Reserves are thus built up at the new insurer as well, which cannot be allocated to healthcare, along with the solvency enrichment at the outgoing insurer. I refer to this as inequitable system money. While it is indeed money that the health insurer can use to implement innovations, it is not necessarily allocated for that purpose and was never intended for it.
Only about 3% of all healthcare costs in the Netherlands go towards the organizational costs of health insurers. These reserves likely fall under this category; nevertheless, they could have been funds spent directly on healthcare under a different systematic approach. If it now turns out that healthcare steering based on the different policies of insurers is undesirable, and that inequitable system funds are indeed such, it raises the question for me as to why there are different health insurance parties. Especially since these elements touch upon the principles of the system. Healthcare steering affects accessibility and quality, while system funds impact affordability. What advantage is there then? I will return to this shortly regarding the challenges surrounding the implementation of the Integral Care Agreement (IZA).
Accessibility
The accessibility of healthcare is increasingly under pressure. The capacity in healthcare is declining due to, among other factors, a tight labor market. This tightness is expected to increase in the coming years, while the demand for healthcare continues to rise. This creates a diverging picture in problem-solving. It requires aligning both variables in such a way that we can tackle the issue of accessibility.
Rising waiting times, more intensive interventions due to delayed treatment, etc. These examples are already painfully visible within mental healthcare and are increasingly coming into focus in specialized medical hospital care.
It is important to examine where the catalyst of this problem lies. In recent years, the healthcare covered by the basic health insurance package (ZVW) has only increased in volume. This variable also poorly relates to capacity and demand for care. More explicit choices could and should be made in this regard. Improvements in medical technology or innovative surgical procedures should only be eligible for reimbursement if they:
- scientifically and/or empirically proven to be medically (cost) effective;
- proven to increase the chance of recovery;
- reduce the (total) societal healthcare costs;
- enhance the quality of life in combination with the associated societal benefits.
This last aspect is indeed particularly difficult to shape, but it is existential to the entire discussion of why medical healthcare exists at all. I see the government as having been largely unsuccessful in making those choices in recent years. It requires making package choices or engaging in existential and ethical discussions. As long as one continues to push that hot potato away and accepts an ever-increasing share of what is possible in terms of medical support, placing it with the increasingly tightening healthcare production apparatus, the ability to provide the necessary care becomes ever smaller.
Insurers, on the other hand, have had more success in this discussion, but in my view, the government’s backing on this issue is largely lacking. The government should take the lead in weighing the above variables much more. To facilitate those difficult choices and accommodate the weighing of that multi-headed discussion monster, the healthcare institute should be the main player. They have not been able to fulfill this role adequately due to the lack of political backbone from the national government, which results in insurers being unfairly labeled as bothersome and parasitic. The mandate they have is simply no longer appropriate.
Only in the current cabinet period do we see the discussion becoming more explicit about the concentration of complex and expensive care; consider the discussion about pediatric cardiology. This discussion is then quickly held hostage by an insufficiently balanced stance (as confirmed by the NZA). It seems that much lobbying has been decisive for the choice, where content should have been the driver of the decision.
This mechanism reveals that politics has a significant influence on healthcare. This is the same healthcare intended to function as a market in the current system. Partly, that market has come into being. This means that there is ample entrepreneurship. Many specialists have felt the need to focus on specific care offerings; and with success. This creates freedom of choice and thus accessibility, and it brings the concomitant effect that the focus increases quality. The protectionist intervention from the government, on the other hand, remains present in the market, and it is questionable whether the system is suitable for that. Who is the government to not apply inflow regulation on technological innovation, yet to have opinions on the rates that can be maximally charged in the ICU? Rates that may subsequently be insufficiently covering and where the affordability of those products must be supplemented by the revenues from elective care. Meanwhile, hospitals themselves must keep their finances in check regarding profit and loss. I find that a particularly troubling principle. The government seems to be able to intervene too arbitrarily because the importance of healthcare is so tremendously great for the BV Nederland. There needs to be more explicit determination of where intervention is allowed and occurs, and where it is not. There should be clearer guidelines established in advance.
Transformation of care and the awaiting challenges
For years, the sector has dealt with the governance framework agreement (HLA). With the potential threat of the macro management instrument (MBI) being implemented, the total sum of specialized medical care was "curbed." In 2022, a successor to the HLA finally emerged with the introduction of the integral healthcare agreement. An agreement that primarily focuses on collaboration within the sector. I believe this is a positive development. As previously outlined, there are cost prices present in the market, there are no longer extreme excesses due to cost unknowns, and the rates are reasonably aligned. The healthcare landscape looks very different now compared to when the current system was introduced in 2006.
However, collaboration is akin to high-performance sports. For many healthcare organizations (especially those with many multi-disciplinary teams), it is already challenging enough to stay on course and keep all the "frogs in the wheelbarrow." Let alone to broaden this to include collaboration with more organizations. I won't even start discussing the strict limitations of payment titles.
To stimulate and ensure successful collaboration, I believe that several variables, as we currently know them, need to be reconsidered. Otherwise, it is doomed to fail in achieving the transformation mentioned in the IZA. The government has responded well by allocating a transformation budget. Funds to ensure that innovation can be established that leads to sustainable, adequate, and efficiently interconnected care. Additionally, placing market-leading insurers in the lead to evaluate innovation policies is very effective. Are we subtly moving back towards representation? But then what?
Once an initiative is developed and the proof-of-the-pudding of the initiative wants to embed the results within the organization, there must be a sustainable payment title in place. Where price pressure is still disproportionately high, access to care is under strain, and not everyone shares the same interest in making quality transparent, this becomes quite a complex issue. Would it not be much more desirable to link this transformation to those who commit to this innovation (regardless of the type of care) also taking the development of a sustainable payment title into account? That would, in my view, be a no-brainer. This would empower the parties involved where they currently see barriers. These barriers may differ per collaboration, but those who take action now should certainly serve as ambassadors for the sector. How can collaboration continue on a smoothly paved floor once the initiative phase is over? Help the collaborating organizations to be compensated according to their own funding proposals, as long as it aligns with the principles of the system with which I began my argument.
I would not suggest completely turning the current healthcare system upside down. Based on the ambassadors who are now emerging as innovative forces in the market, I would draw lessons from what works. I would propose that the system be adjusted iteratively and that, over time, broadening is found. This aligns with the idea of appreciative inquiry; what were the real keys to success? What should we continue doing today, what should we start doing tomorrow, and what should we definitely stop doing because it does not help us?
But well, that remains merely my perspective on the matter. Please feel free to let me know if you would like to exchange thoughts on this; I would love that!
Best regards,